Vitamin D supplementation could possibly improve clinical outcomes of patients infected with Coronavirus-2019 (Covid- 2019)
Mark M. Alipio April 9, 2020
Department of Radiologic Technology, College of Allied Health Sciences, Davao Doctors College
Gen. Malvar St., Davao City 8000, Davao del Sur, Philippines, Office +63 (082) 222 0850, markalipiorrt at gmail.com
Chart of data by GrassrootsHealth
Chart of data in German VitaminDService
German vertical axis is the number of people in each group, GRH vertical axis is a % of 100%
To the Editor:
The rapid spread of Covid-2019 in many areas of the world calls for preventive health measures. Although basic guidelines on infection control are recommended, treatment has remained the best choice to avert mortality. However, for the time being, there are no known vaccines for the disease. This has driven several researchers in the world to assess the effectiveness of previously used treatments for severe acute respiratory syndrome (SARS) such as lopinavir.1 Clinical trials for these vaccines could take more time, hence, palliative drugs have been developed to alleviate the severity of the disease.
Vitamin D has been proven to reduce risk of getting common cold.2 It also enhances cellular immunity,3 modulates adaptive immunity,4 and enhances expression of antioxidation-related genes.5 Hence, several authors proposed Vitamin D supplementation to prevent and treat Covid- 2019.6,7,8 To the best of my knowledge, no clinical trials have been conducted yet to determine the potency of Vitamin D in suppressing SARS-CoV-2 strain. A statistical analysis of the association between Vitamin D levels and clinical outcomes of Covid-2019 patients has not been described. In this paper, I used multinomial logistic regression to predict clinical outcomes of patients infected with Covid-2019 based on 25-hydroxyvitamin D [25(OH)D] levels, the barometer for Vitamin D status.
Using the database of three hospitals in Southern Asian countries, I conducted a retrospective multicentre study of 212 cases with laboratory-confirmed infection of SARS-CoV-2. Data pertaining to clinical features and serum 25(OH)D levels were extracted from the medical records. No other patient information was provided to ensure confidentiality. I classified the cases as follows: (1) mild - mild clinical features without pneumonia diagnosis, (2) ordinary - confirmed pneumonia in chest computer tomography with fever and other respiratory symptoms, (3) severe
-hypoxia (at most 93% oxygen saturation) and respiratory distress or abnormal blood gas analysis results (PaC〇2 >50 mm Hg or Pa〇2 < 0 mm Hg), and (4) critical - respiratory failure requiring intensive case monitoring. Classification was based on a previous work.9 I also classified the vitamin D status of the cases based on their serum 25(OH)D level: (1) normal - 25(OH)D of > 30 ng/ml, (2) insufficient - 25(OH)D of 21-29 ng/ml, and (3) deficient - 25(OH)D of < 20 ng/ml.
A previous report guided this classification.10 For statistical analysis, I used Mann-Whitney U and x2 tests to compare differences in the clinical outcomes. Multinomial logistic regression was used to explore the association between serum 25(OH)D level and clinical outcomes of the cases. Frequency and percentage were used for categorical variables. Mean was used for continuous variables. A p-value below 0.01 was considered statistically significant. Ethics approval was considered exempt owing to the nature of the study and open-access data used. All names were originally hidden by the health governing bodies to ensure patient confidentiality.
Table 1. Descriptive statistics
Note: OR = odds ratio associated with the effect of a one standard deviation increase in the predictor.
Table 2. Multinomial logistic regression analysis
Of the 212 (100.0%) cases of Covid-2019, 49 (23.1%) were identified mild, 59 (27.8%) were ordinary, 56 (26.4%) were severe, and 48 (22.6%) were critical (Table 1). Mean serum (OH)D level was 23.8 ng/ml. Serum (OH)D level of cases with mild outcome was 31.2 ng/ml, 27.4 ng/ml for ordinary, 21.2 ng/ml for severe, and 17.1 ng/ml for critical. Serum (OH)D levels were statistically significant among clinical outcomes (p<0.001). A total of 55 (25.9%) cases had normal Vitamin D status, majority of which (85.5%) were identified mild. A total of 80 (37.7%) cases had insufficient Vitamin D status, majority of which (43.8%) were ordinary. Cases identified as Vitamin D-deficient were 77 (36.3%), majority of which were severe (40.3%).
Vitamin D status is significantly associated with clinical outcomes (p<0.001).
A multinomial logistic regression analysis reported that the odds of having a mild clinical outcome rather than an ordinary outcome were approximately 1.63 times (OR=0.614, p=0.007) for each standard deviation increase in serum (OH)D (Table 2).
Also, for each standard deviation increase in serum (OH)D, the odds of having a mild clinical outcome rather than a severe outcome were approximately 7.94 times (OR=0.126, p<0.001) while interestingly, the odds of having a mild clinical outcome rather than a critical outcome were approximately more than 19.61 times (OR=0.051, p<0.001).
More generally, the odds of having a mild clinical outcome increase when serum (OH)D level increases. Alternatively, the odds of having a critical outcome increase when serum (OH)D level decreases. This means that serum (OH)D level in the body could account for the clinical outcomes of the patients infected with Covid-2019. An increase in serum (OH)D level in the body could either improve clinical outcomes or mitigate worst (severe to critical) outcomes. On the other hand, a decrease in serum (OH)D level in the body could worsen clinical outcomes of Covid-2019 patients. In this case, Vitamin D supplementation may play an important role to raise 1,25- dihydroxyvitamin D [1,25(OH)2D], the biologically active form of Vitamin D in the blood.
In conclusion this study provides substantial information to clinicians and health policy-makers. Vitamin D supplementation could possibly improve clinical outcomes of patients infected with Covid-2019 based on increasing odds ratio of having a mild outcome when serum (OH)D level increases. Further research may conduct randomized controlled trials and large population studies to evaluate this recommendation.
References
- Sohrabi, C., Alsafi, Z., ONeiU, N., Khan, M., Kerwan, A., Al-Jabir, A., ... & Agha, R. (2020). World Health Organization declares global emergency: A review of the 2019 novel coronavirus (COVJD-19). International Journal of Surger
- Lei, G. S., Zhang, C., Cheng, B. H., & Lee, C. H. (2017). Mechanisms of action of vitamin D as supplemental therapy for Pneumocystis pneumonia. Antimicrobial agents and chemotherapy, 61(10), e01226-17. y.
- Rondanelli, M., Miccono, A., Lamburghini, S., Avanzato, I., Riva, A., Allegrini, P., ... & Perna, S. (2018). Self-care for common colds: the pivotal role of vitamin D, vitamin C, zinc, and Echinacea in three main immune interactive clusters (physical barriers, innate and adaptive immunity) involved during an episode of common colds 一Practical advice on dosages and on the time to take these nutrients/botanicals in order to prevent or treat common colds. Evidence-Based Complementary and Alternative Medicine, 2018.
- Cantorna, M. T. (2010). Mechanisms underlying the effect of vitamin D on the immune system. Proceedings of the Nutrition Society, 69(3), 286-289.
- Sharifi, A., Vahedi, H., Nedjat, S., Rafiei, H., & Hosseinzadeh-Attar, M. J. (2019). Effect of single-dose injection of vitamin D on immune cytokines in ulcerative colitis patients: a randomized placebo-controlled trial. Apmis, 127(10), 681-687.
- Wimalawansa, S. J. (2020). Global epidemic of coronavirus--COVID-19: What we can do to minimize risks. European XXXXX, 7(3), 432-438.
- Grant, W. B., Lahore, H., McDonnell, S. L., Baggerly, C. A., French, C. B., Aliano, J. L., & Bhattoa, H. P. (2020). Evidence that Vitamin D Supplementation Could Reduce Risk of Influenza and COVID-19 Infections and Deaths.姓/rien/s, 12(4), 988.
- Braiman, M. (2020). Latitude Dependence of the COVID-19 Mortality Rate—A Possible Relationship to Vitamin D Deficiency?. Axx mlable at SSRN3561958.
- Wang, Y., Liu, Y., Liu, L., Wang, X., Luo, N., & Ling, L. (2020). Clinical outcome of 55 asymptomatic cases at the time of hospital admission infected with SARS-Coronavirus-2 in Shenzhen, China. The Journal of infectious diseases.
- Holick, M. F. (2009). Vitamin D status: measurement, interpretation, and clinical application. Annals of epidemiology, 19(2), 73-78.
COVID-19 treated by Vitamin D - studies, reports, videos
As of March 31, 2024, the Vitamin D Life COVID page had: trial results, meta-analyses and reviews, Mortality studies see related: Governments, HealthProblems, Hospitals, Dark Skins, All 26 COVID risk factors are associated with low Vit D, Fight COVID-19 with 50K Vit D weekly Vaccines Take lots of Vitamin D at first signs of COVID 166 COVID Clinical Trials using Vitamin D (Aug 2023) Prevent a COVID death: 9 dollars of Vitamin D or 900,000 dollars of vaccine - Aug 2023
5 most-recently changed Virus entries
Recent COVID-19 articles Click here for all VIRUS articles on Vitamin D Life
- COVID fought by Vitamin D: 2.3X less likely to die of COVID if supplemented, 1.9 X less likely to become infected – meta-analysis March 2024
- US has the most vaccinations before age 1 and the most deaths - March 2024
- Benign Cancers of a portion of the brain increased 1.8 X after vaccines were available - March 2024
- Long-COVID 3.1 X more likely if insufficient amounts of Magnesium and Vitamin D – March 2024
- COVID US survey: 43% not expect to ever return to normal – Gallup March 2024
- COVID-19 leaves its mark on the brain, dropping in IQs - March 2024
- 100% not need COVID hospitalization with fluvoxamine plus one other drug – Thailand RCT April 2024
- COVID maximum downregulation of Vitamin D receptor and CYP27B1 resulted in death - Feb 2024
- COVID-19 vaccines adverse events: myocarditis, pericarditis, etc. (99 million people, not US) – Feb 2024
- COVID could have been stopped in Wuhan – book March 2024
- Vitamin D: Viral infections, Infectious diseases, EBV and MS, Virus and Cancers – Grant March 2024
- Senator Ron Johnson hosted talks on COVID treatments - 2020 - 2024
- COVID infection (without hospitalization) – 1.7X more likely to die in 6 months if low Vitamin D – March 2024
- COVID senior pneumonia deaths: 50% if low Vitamin D and unvaccinated vs 16% if Vitamin D or vaccinated – June 2023
- 5 X less COVID infection of health care workers who took lots of vitamin D – meta-analysis Feb 2024
- 18,000 schoolchildren in Canada to be suspended for not being vaccinated - Feb 2024
- Vaccines increased your risk of dying of COVID in NZ - official data - Feb 2024
- Study urged a global moratorium on mRNA vaccines (300 peer reviewers agreed) – Jan 2024
- CDC recommends 100 vaccinations by age 18 – Feb 2024
- Professor Raoult is calling for a moratorium on COVID-19 vaccines - Jan 2024
- COVID deaths cut in half by a single dose of 600,000 IU of Vitamin D - RCT Jan 2024
- Is 50 ng of Vitamin D enough to fight COVID - TrialSiteNews - Jan 2024
- COVID and or vaccinations causing less Vitamin D and more sickness - Jan 2024
- Long-COVID a month shorter if more than 20 ng of Vitamin D - Jan 2024
- COVID, Vitamin D, Drs. Grimes and Campbell - Jan 2024
- All died of COVID with standard vitamin D, 25% survived if 10X more vitamin D (mice) – Dec 2023
- COVID infections and vaccinations decrease Vitamin D – many studies
- Moderna is monitoring 150 million websites for ‘Anti-Vaccine’ Narratives - Nov 2023
- But not Vitamin D Life, so far
- The four viruses that are increasing at an ‘exponential rate’ (are all fought by Vitamin D) – Nov 2023
- COVID death rate 4X less at high altitude (more UVB which makes Vitamin D) - Oct 2023
- Doctors in NY cannot opt out of COVID boosters for children - Oct 2023
- Multiple COVID vaccinations might increase Cancer Incidence - many studies
- COVID fought by Vitamin D - video review of literature with transcript - Dec 2021
- What to do if you catch COVID - Dr. McCullough Sept 2023
- Long COVID with Neuro-Cognitive symptoms had especially low vitamin D levels – Sept 2023
- Mask studies for viral infection: 104 studies: ineffective, 61 studies: harmful - Sept 2023
- The ONLY Solution to Long COVID (Vitamin D) - video and transcript Sept 2023
- Long-COVID can hide in the body for years in scores of locations – Sept 2023
- Vaccine Clinical Trial - cardiovascular death 3.7X more likely if vaccinated - preprint Sept 2023
- One in five people with long COVID can no longer work (Doctors in this case) - Sept 2023
- Number of people with long COVID could be vastly underestimated - Aug 2023
- mRNA Vaccine Toxicity -free book by Doctors for COVID Ethics - Aug 2023
- Politics says put your masks back on, Science says masks may INCREASE COVID infection - Aug 2023
- Epstein-Barr Virus may be a prerequisite for Multiple Sclerosis - July 2023
- COVID Vaccinations increased risk of cardiac deaths in youths by 19% - Aug 2023
- Athletes who had been COVID infected had lower Vitamin D levels – July 2023
- Vitamin D was the most popular supplement during the COVID Pandemic – July 2023
- COVID cost the US 18,000 dollars per survivor, and many excess deaths - July 2023
- COVID, Long-COVID and Vitamin D in children - Review April 2023
- COVID in hospital stopped by Vitamin D Receptor activators (curcumin, quercetin) – RCT June 2023
- Children with COVID 4X more likely to have poor Vitamin D Receptors (Note: COVID deactivates VDR) – April 2023
- Chance of moderately severe COVID 3X less likely if plant-based diet – April 2021
- COVID, Long COVID, and Vitamin D – May 2023
- 3,400 peer-reviewed studies found COVID Vaccination problems as of April 2023
- COVID death 1.5 X less likely if high vitamin D, emergency D (50K to 100K) is great – meta-analysis March 2023
- Poor vaccine batches associated with adverse events - March 2023
- Probably less of a problem if had high Vitamin D when vaccinated
- Excess deaths - 5 possible reasons - many studies
- COVID was associated with low Vitamin D or Zinc – umbrella review Feb 2023
- COVID predicted to be a pandemic that could be stopped by high dose vitamin D - Feb 2020
- COVID and other Virus fought by UV - many studies
- Seniors raised Vitamin D levels, more COVID survivors, less CKD (Slovakia) – Feb 2023
- COVID recovery 1.6X faster after 200,000 IU of Vitamin D RCT – Feb 2023
- Multisystem Inflammatory Syndrome of COVID in Children 3X more likely if low Vitamin D – Feb 2023
- COVID was associated with low Vitamin D or Zinc – umbrella review Feb 2023
- Vitamin D, now conclusive (for COVID) - Dr. Campbell Video and transcript - Feb 1, 2023
- COVID ICU 3X less-likely if take any amount and type of Vitamin D – meta-analysis Jan 2023
- 2nd COVID infection increases the risk of Long-COVID - 2022
- More COVID vaccinations, more infections - Cleveland Clinic - Dec 2022
- COVID vaccination increased by 137X the risk of 10-14 year olds of dying (UK) – Jan 2023
- Chart of excess deaths and vaccination in the Netherlands - for 2022
- China: From Zero Covid to No Plan - people left to improvise - NYT Dec 18, 2022
- COVID variants in US evade bivalent vaccination by 3X to 13X – Cell Dec 13, 2022
- Fight infections such as COVID with 50 ng of Vitamin D – Sunil Dec 2022
- COVID and Vitamin D: any amount of D, at any time, for any duration reduced ICU - meta-analysis Dec 2022
- The vitamins and minerals that help the immune system respond to respiratory viruses – Dec 2022
Intervention
Intervention Trial Summary Table
Details on #5 = COVIT-TRIAL Dec 27
Note: >70% of the RCT using Vitamin D to fight COVID-19 are using at least 100,000 IU during the first week
Trial Results 43 studies in both Virus and InterventionThis list is automatically updated
- 5 X less COVID infection of health care workers who took lots of vitamin D – meta-analysis Feb 2024
- COVID deaths cut in half by a single dose of 600,000 IU of Vitamin D - RCT Jan 2024
- COVID in hospital stopped by Vitamin D Receptor activators (curcumin, quercetin) – RCT June 2023
- Vitamin D Supplements Don’t Reduce COVID-19 Risk (used only 3,200 IU daily) - Oct 2022
- High dose vitamin D fights Folate gene changes by COVID, autoimmune, CVD, ALZ – Oct 2022
- COVID in hospital fought by Vitamin D (25,000 IU daily for 4 days, then 25K weekly) - RCT – July 2022
- Small Vitamin D doses for a short time never help (not improve vaccination in this case) – RCT Sept 2022
- The challenges of a Vitamin D RCT – too many already taking it, etc. – Martineau Sept 2022
- Early COVID treatments rarely work 7 days after symptoms, this trial gave Vitamin D on 7th day – RCT May 2022
- COVID children helped by Vitamin D, trial terminated: unethical to not give Vitamin D to all: – RCT July 2022
- COVID hospital deaths reduced 2X by 8 days of UVB – pilot RCT May 2022
- 21 fewer days in hospital with ARDS (COVID) if 10,000 IU of Vitamin D daily after enter hospital – RCT April, 2022
- 4X less likely to get COVID following 4,000 IU daily for a month – RCT April 2022
- Risk of COVID not reduced by 3,200 IU of vitamin D during 6 months (no surprise) – RCT March 2022
- Group achieving 30 ng (vs 26 ng) were 2X less likely to get COVID symptoms - RCT Jan 2022
- Tested positive for COVID, taking probiotics stopped symptoms 5 days sooner - RCT Jan 2022
- Vitamin D given slowly in hospital did not fight COVID-19 much - Nov 2021
- Nursing home vaccinated against Influenza, 800 IU of vitamin D daily cut infection rate in half – small RCT Oct 2021
- COVID-19 appears reduced by Resveratrol plus 100K IU of vitamin D – Small RCT Sept 2021
- Vitamin D trial for COVID-19 – using their patented slow-release form – Aug 2021
- COVID-19 mortality reduced 4X (chart looks like 2X) by large, infrequent doses of Vitamin D in France – July 2021
- COVID-19 outpatients getting Quercetin nanoemulsion had excellent outcomes (Q increased Vitamin D in cells) – RCT – June 2021
- 5,000 U daily raised Vitamin D a bit and helped COVID-19 a bit – RCT June 2021
- COVID-19 inflammation extinguished by 60,000 IU of vitamin D nanoemulsion daily for a week – RCT May 2021
- Better response to shingles virus after 6,400 IU Vitamin D raised above 40 ng – Jan 2021
- COVID-19 ICU survival rate increased 7X by daily Omega-3 – RCT March 2021
- Kidney patients who happened to be getting high-dose Calcitriol were 9X less likely to die of COVID-19 - April 6, 2021
- Vitamin D not help 10 days after COVID-19 symptoms - RCT March 2021
- 5X less likely to enter ICU with COVID-19 if get Calcifediol (semi-activated vitamin D) - RCT Feb 19, 2021
- calcifediol rct
- COVID-19 defeated 3x faster by 420,000 IU Vitamin D nanoemulsion – RCT Nov 12, 2020
- COVID-19 defeated by calcifediol form of Vitamin D in Spain - pilot RCT Aug 29, 2020
- Swine flu not prevented by 2,000 IU of vitamin D daily (the upper limit at the time) – RCT 2014
- Influenza vaccine antibodies not change with Vitamin D – 21 ng or 44 ng – RCT Feb 2019
- Dengue virus prevented by a small amount of Vitamin D – RCT Nov 2019
- Half the risk of Influenza -A in infants taking 1200 IU of vitamin D for 4 months – RCT Jan 2018
- Chikungunya virus arthritis pain reduced by weekly 60,000 IU vitamin D – Sept 2016
- Many Infectious diseases (virus) treated and prevented by Vitamin D – review July 2009
- Influenza prevented by 40 ng levels or treated with vitamin D hammer (50,000 IU) – June 2015
- Infection fighting ability increased with 5,000 IU Vitamin D daily – April 2015
- Vitamin D prevents Hepatitis-C and helps treat it (many studies)
- Malaria in mice brains, and associated inflammation, prevented by Vitamin D intervention – July 2014
- Influenza A: 5X reduction in first month (only) with 2,000 IU of vitamin D– RCT July 2014
Virus meta-analyses and Systematic Reviews
Short URL for this section = is.gd/vdwmeta
- COVID fought by Vitamin D: 2.3X less likely to die of COVID if supplemented, 1.9 X less likely to become infected – meta-analysis March 2024
- COVID Vaccinations increased risk of cardiac deaths in youths by 19% - Aug 2023
- T1 Diabetes increased by 27% by second year of COVID – meta-analysis June 2023
- Yet another reason to take Vitamin D while pregnant – fight COVID - meta-analysis May 2023
- COVID death 1.5 X less likely if high vitamin D, emergency D (50K to 100K) is great – meta-analysis March 2023
- COVID ICU 3X less-likely if take any amount and type of Vitamin D – meta-analysis Jan 2023
- COVID and Vitamin D: any amount of D, at any time, for any duration reduced ICU - meta-analysis Dec 2022
- Worse COVID during 3Q pregnancy if 2.5 ng lower Vitamin D – meta-analysis Sept 2022
- Severe COVID 2.6 X less likely if supplement with Vitamin D – 26th meta-analysis - July 2022
- COVID Long-Haul prevalence increases with time: 50% at 4 months - meta June 2022
- COVID test positive is about half as likely if have Vitamin D – 24th meta-analysis - Jan 2022
- Small amounts of Vitamin D reduce Influenza risk by 22 percent (loading dose is far better) – meta-analysis Jan 2022
- Vitamin D fights COVID (54 studies of 1,400,000 people) – 23rd meta-analysis - Dec 2021
- COVID-19 treated by Vitamin D (reduce ICU by 3X) - 22nd meta-analysis - Dec 29, 2021
- COVID-19 death increased 2X if low Vitamin D (less than 10 to less than 30 ng) – 21st meta-analysis Dec 2021
- COVID-19 risk reduced by vitamin D supplementation – umbrella review of 7 meta-analysis – Oct 2021
- COVID-19 treated by Vitamin D (example: ICU reduced by 5X) – 20th meta-analysis Oct 13, 2021
- Severe COVID-19 2.5 X more likely if low vitamin D (23 studies) – 19th meta-analysis Oct 2021
- COVID-19 mortality extrapolates to zero at 50 ng of vitamin D – 18th Meta-analysis Sept 2021
- COVID-19 death 1.6 X more likely if low vitamin D (24 studies) – 17th meta-analysis Aug 2021
- Severe COVID-19 5X more likely if low vitamin D (23 studies) – 16th meta-analysis July 2021
- Severe COVID-19 3.5 more likely if low vitamin D (30 studies) – meta-analysis July 2021
- COVID-19 patients who had supplemented with Vitamin D were 3X less likely to enter ICU – June 2021
- Low Calcium associated with severe COVID-19 – several studies
- COVID-19 mortality 3X more likely if low vitamin D (999,179 people) – meta-analysis March 29, 2021
- COVID-19 was 2.6X more severe if very low Vitamin D (43 studies) – meta-analysis March 26, 2021
- Low Vitamin D associated with 2.7X more severe COVID-19 – 12th MA March 5, 2021
- Vitamin D supplementation fights COVID-19 – 11th meta-analysis Jan 24, 2021
- 3.7 X less likely to die of COVID-19 if supplemented with Vitamin D - meta-analysis Jan 5, 2021
- Less likely to test positive for COVID-19 if higher Vitamin D – meta-analysis Jan 6, 2021
- Vitamin D reduces COVID-19 by 80 percent - anonymous meta-analysis - Jan 5, 2021
- COVID-19 1.7X more likely to be severe if low Vitamin D - meta-analysis Oct 2020
- Low Vitamin D associated 1.8X increased risk of COVID-19 death in hospital – meta-analysis Nov 4, 2020
- Acute viral respiratory infections (RTI) reduced by Vitamin D - 20 reviews - Aug 2020
- Prudent to consider that Vitamin D has a role in COVID-19 – meta-analysis – Aug 7, 2020
- Risk of enveloped virus infection is increased 50 percent if poor Vitamin D Receptor - meta-analysis Dec 2018
- Hepatitis B patients have 2 ng lower level of Vitamin D – meta-analysis June 2019
- Influenza Vaccination not benefited by lowish levels of vitamin D – meta-analysis March 2018
Reviews
- Vitamin D supplementation reduced risk of COVID-19 ICU by 2.8 X – review of 10 reviews Feb 2022
- COVID-19 and Vitamin D (42 studies, consensus) – Oct 2021
Observe - Less likely to become infected
short URL to this section = https://is.gd/COVID_less
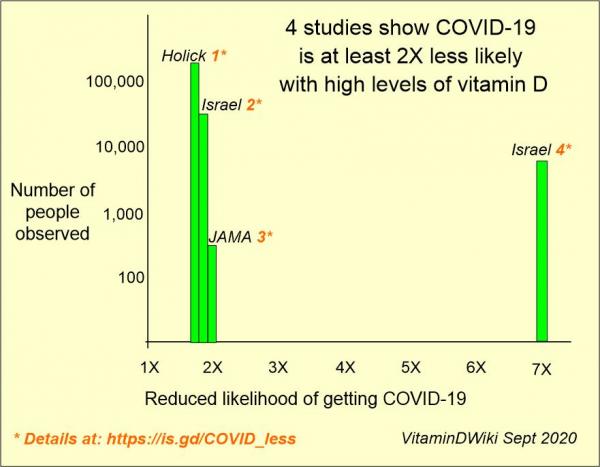
- 14 X less likely to have severe COVID if previously had more than 40 ng level of Vitamin D – Feb 2022
- COVID-19 patients had low levels of Zinc, Vitamin A, Vitamin D, and Vitamin C – Sept 2021
Observe - Reduced Severity/Death
MORTALITY AND Virus (automatically updated):
- Moderna report: their COVID vax caused "only" 17,751 deaths - April 2024
- COVID infection (without hospitalization) – 1.7X more likely to die in 6 months if low Vitamin D – March 2024
- Vaccines increased your risk of dying of COVID in NZ - official data - Feb 2024
- 3X increase in unspecified causes of Death (Canada 2019-2022) - Dec 2023
- Deaths after vaccination - also reported in Japan - Dec 2023
- Excess deaths after COVID vaccination - 17 countries - Sept 2023
- Excess Deaths in Australia jumped up in 2022– preprint Feb 2023
- Prevent a COVID death: 9 dollars of Vitamin D or 900,000 dollars of vaccine - Aug 2023
- Number needed to vaccinate to prevent 1 Omicron death: 30,000 for age 60-70 - Sept 2022
- COVID survival in Europe in 2020 best predicted by population-level Vitamin D (of 13 variables) – July 2022
- Elderly who had been in COVID ICU were 4X more likely to die if low vitamin D – Nov 2022
- More COVID mortality if less than 20 ng of Vitamin D (Mexico) – May 2022
- 15,000,000 excess deaths in 2 years - May 2022
- COVID death 5.2X more likely if Vitamin D deficient – May 2022
- 29 X more likely to die of COVID if less than 20 ng of Vitamin D - March 2022
- Giving Vitamin D reduced COVID Mortality– Review of 11 studies – March 2022
- 18 million excess global deaths in past 2 years: COVID plus collateral damage - Lancet March 2022
- COVID severity and death more likely if low vitamin D (Egypt this time) - March 2022
- US nursing homes are epicenters for COVID deaths (200,000) - Feb 2022
- Ivermectin taken before COVID decreased death rate by 68 percent (3,000 with Ivermectin vs 3,000 without) - Dec 24, 2021
- Increase in non-COVID deaths (ages 18-64) in Indiana, India, etc. - Jan 5, 2022
- Only 35,000 died in US of COVID who previously had been healthy
- COVID-19 mortality extrapolates to zero at 50 ng of vitamin D – 18th Meta-analysis Sept 2021
- COVID-19 patients getting 300,000 IU of Vitamin D were 5X less likely to die – Sept 2021
- Predict 2X more likely to die of COVID-19 if vitamin D Deficient (Iran 2020) – Sept 2021
- COVID-19 mortality not associated with Vitamin D (everyone had very low levels) -Sept 2021
- COVID-19 mortality for Blacks is 5X that for whites in 2 LA Hospitals - July 2021
- COVID-19 mortality was associated with vitamin D deficiency of 47 countries – July 2021
- Similar death rate for Vaccination and COVID-19 study and video – June 24, 2021
- COVID-19 death in hospital 5X more likely if low vs high vitamin D – preprint June 2021
- COVID-19 deaths 1.7X more likely if low vitamin D (even after “adjusting” for low D health problems) – May 2021
- COVID-19 deaths 1.5X less likely if more than 40 ng of vitamin D – US VA – April 2021
- Vitamin D supplementation and high levels reduce COVID-19 deaths in elderly – Review April 17, 2021
- Less COVID-19 infection, mortality in countries with higher Vitamin D (Asia in this case) – May 2021
- COVID-19 was the third-leading cause of death in the US, especially in those with dark skins - April 1, 2021
- Risk of COVID-19 death was 4.9 X higher if very low vitamin D – March 31, 2021
- COVID-19 mortality 2X higher if low Vitamin D (Mexican hospital, preprint) - March 2021
- All COVID-19 patients had low vitamin D, the lowest were more likely to die – Feb 18, 2021
- 2.7 fewer COVID-19 hospital deaths in those having more than 30 ng of vitamin D – Mayo Jan 9, 2021
- Worse COVID-19 patients got 400,000 IU of vitamin D, deaths cut in half – Jan 14, 2021
- Iranians with COVID-19 were 2.3 X more likely to die if low vitamin D – Jan 2021
- Poor COVID-19 prognosis was 6 X more likely if low vitamin D – Jan 21, 2021
- Less than 10 dollars of Vitamin D per COVID-19 life saved in Myanmar - Jan 2021
- 2.8 X fewer COVID-19 nursing home deaths if add 10,000 IU Vitamin D daily for a week (small observation)- Jan 2021
- Italian nursing home COVID-19 – 4X less likely to die if taking Vitamin D– Dec 22, 2020
- Shift workers 2X more likely to get COVID-19 (low Vitamin D) - Dec 2020
- Those getting high dose vitamin D were 7 X less likely to die of COVID-19 - Dec 11, 2020
- COVID-19 male mortality increased 3.9 X if low vitamin D – observation Nov 25, 2020
- Hospital COVID-19 observation: 7X more likely to live if more than 20 ng of vitamin D– Nov 19, 2020
- COVID-19 lung death 4X more likely in Iran if less than 25 ng of vitamin D – Oct 30, 2020
- Vitamin D of 30-40 ng fights COVID, Dr. Grimes on Liverpool Study - March 2022
- Higher vitamin D, less severe COVID and deaths in hospital (in Iran this time) – Sept 2021
Vitamin D Dosing Recommendations for COVID-19
- COVID predicted to be a pandemic that could be stopped by high dose vitamin D - Feb 2020
- FLCCC COVID guidelines now include vitamin D loading doses - Jan 2022
- Vitamin D and COVID, review of evidence, loading dose if less than 50 ng - Masterjohn Sept 2021
Short URL for this section = https://is.gd/covitamind https://is.gd/virusvitd
Title change made in Sept 2022 caused the visitor count to reset.
There have actually been 120630 visitors to this page since it was originally made
COVID-19 was 19X more likely if low vitamin D (may be invalid data)– April 2020 7269 visitors, last modified 04 Jul, 2020,
Printer Friendly Follow this page for updates This page is in the following categories (# of items in each category) Attached files
ID Name Uploaded Size Downloads 13772 German 19X.jpg admin 29 Apr, 2020 54.42 Kb 5960 13759 Alipio chart.jpg admin 22 Apr, 2020 88.17 Kb 13263 13745 table 2.jpg admin 18 Apr, 2020 15.40 Kb 4427 13744 COVID-19 and Vitamin D deficiency.jpg admin 18 Apr, 2020 58.06 Kb 4799
This list is automatically updated
- 5 X less COVID infection of health care workers who took lots of vitamin D – meta-analysis Feb 2024
- COVID deaths cut in half by a single dose of 600,000 IU of Vitamin D - RCT Jan 2024
- COVID in hospital stopped by Vitamin D Receptor activators (curcumin, quercetin) – RCT June 2023
- Vitamin D Supplements Don’t Reduce COVID-19 Risk (used only 3,200 IU daily) - Oct 2022
- High dose vitamin D fights Folate gene changes by COVID, autoimmune, CVD, ALZ – Oct 2022
- COVID in hospital fought by Vitamin D (25,000 IU daily for 4 days, then 25K weekly) - RCT – July 2022
- Small Vitamin D doses for a short time never help (not improve vaccination in this case) – RCT Sept 2022
- The challenges of a Vitamin D RCT – too many already taking it, etc. – Martineau Sept 2022
- Early COVID treatments rarely work 7 days after symptoms, this trial gave Vitamin D on 7th day – RCT May 2022
- COVID children helped by Vitamin D, trial terminated: unethical to not give Vitamin D to all: – RCT July 2022
- COVID hospital deaths reduced 2X by 8 days of UVB – pilot RCT May 2022
- 21 fewer days in hospital with ARDS (COVID) if 10,000 IU of Vitamin D daily after enter hospital – RCT April, 2022
- 4X less likely to get COVID following 4,000 IU daily for a month – RCT April 2022
- Risk of COVID not reduced by 3,200 IU of vitamin D during 6 months (no surprise) – RCT March 2022
- Group achieving 30 ng (vs 26 ng) were 2X less likely to get COVID symptoms - RCT Jan 2022
- Tested positive for COVID, taking probiotics stopped symptoms 5 days sooner - RCT Jan 2022
- Vitamin D given slowly in hospital did not fight COVID-19 much - Nov 2021
- Nursing home vaccinated against Influenza, 800 IU of vitamin D daily cut infection rate in half – small RCT Oct 2021
- COVID-19 appears reduced by Resveratrol plus 100K IU of vitamin D – Small RCT Sept 2021
- Vitamin D trial for COVID-19 – using their patented slow-release form – Aug 2021
- COVID-19 mortality reduced 4X (chart looks like 2X) by large, infrequent doses of Vitamin D in France – July 2021
- COVID-19 outpatients getting Quercetin nanoemulsion had excellent outcomes (Q increased Vitamin D in cells) – RCT – June 2021
- 5,000 U daily raised Vitamin D a bit and helped COVID-19 a bit – RCT June 2021
- COVID-19 inflammation extinguished by 60,000 IU of vitamin D nanoemulsion daily for a week – RCT May 2021
- Better response to shingles virus after 6,400 IU Vitamin D raised above 40 ng – Jan 2021
- COVID-19 ICU survival rate increased 7X by daily Omega-3 – RCT March 2021
- Kidney patients who happened to be getting high-dose Calcitriol were 9X less likely to die of COVID-19 - April 6, 2021
- Vitamin D not help 10 days after COVID-19 symptoms - RCT March 2021
- 5X less likely to enter ICU with COVID-19 if get Calcifediol (semi-activated vitamin D) - RCT Feb 19, 2021
- calcifediol rct
- COVID-19 defeated 3x faster by 420,000 IU Vitamin D nanoemulsion – RCT Nov 12, 2020
- COVID-19 defeated by calcifediol form of Vitamin D in Spain - pilot RCT Aug 29, 2020
- Swine flu not prevented by 2,000 IU of vitamin D daily (the upper limit at the time) – RCT 2014
- Influenza vaccine antibodies not change with Vitamin D – 21 ng or 44 ng – RCT Feb 2019
- Dengue virus prevented by a small amount of Vitamin D – RCT Nov 2019
- Half the risk of Influenza -A in infants taking 1200 IU of vitamin D for 4 months – RCT Jan 2018
- Chikungunya virus arthritis pain reduced by weekly 60,000 IU vitamin D – Sept 2016
- Many Infectious diseases (virus) treated and prevented by Vitamin D – review July 2009
- Influenza prevented by 40 ng levels or treated with vitamin D hammer (50,000 IU) – June 2015
- Infection fighting ability increased with 5,000 IU Vitamin D daily – April 2015
- Vitamin D prevents Hepatitis-C and helps treat it (many studies)
- Malaria in mice brains, and associated inflammation, prevented by Vitamin D intervention – July 2014
- Influenza A: 5X reduction in first month (only) with 2,000 IU of vitamin D– RCT July 2014
Virus meta-analyses and Systematic Reviews
Short URL for this section = is.gd/vdwmeta
- COVID fought by Vitamin D: 2.3X less likely to die of COVID if supplemented, 1.9 X less likely to become infected – meta-analysis March 2024
- COVID Vaccinations increased risk of cardiac deaths in youths by 19% - Aug 2023
- T1 Diabetes increased by 27% by second year of COVID – meta-analysis June 2023
- Yet another reason to take Vitamin D while pregnant – fight COVID - meta-analysis May 2023
- COVID death 1.5 X less likely if high vitamin D, emergency D (50K to 100K) is great – meta-analysis March 2023
- COVID ICU 3X less-likely if take any amount and type of Vitamin D – meta-analysis Jan 2023
- COVID and Vitamin D: any amount of D, at any time, for any duration reduced ICU - meta-analysis Dec 2022
- Worse COVID during 3Q pregnancy if 2.5 ng lower Vitamin D – meta-analysis Sept 2022
- Severe COVID 2.6 X less likely if supplement with Vitamin D – 26th meta-analysis - July 2022
- COVID Long-Haul prevalence increases with time: 50% at 4 months - meta June 2022
- COVID test positive is about half as likely if have Vitamin D – 24th meta-analysis - Jan 2022
- Small amounts of Vitamin D reduce Influenza risk by 22 percent (loading dose is far better) – meta-analysis Jan 2022
- Vitamin D fights COVID (54 studies of 1,400,000 people) – 23rd meta-analysis - Dec 2021
- COVID-19 treated by Vitamin D (reduce ICU by 3X) - 22nd meta-analysis - Dec 29, 2021
- COVID-19 death increased 2X if low Vitamin D (less than 10 to less than 30 ng) – 21st meta-analysis Dec 2021
- COVID-19 risk reduced by vitamin D supplementation – umbrella review of 7 meta-analysis – Oct 2021
- COVID-19 treated by Vitamin D (example: ICU reduced by 5X) – 20th meta-analysis Oct 13, 2021
- Severe COVID-19 2.5 X more likely if low vitamin D (23 studies) – 19th meta-analysis Oct 2021
- COVID-19 mortality extrapolates to zero at 50 ng of vitamin D – 18th Meta-analysis Sept 2021
- COVID-19 death 1.6 X more likely if low vitamin D (24 studies) – 17th meta-analysis Aug 2021
- Severe COVID-19 5X more likely if low vitamin D (23 studies) – 16th meta-analysis July 2021
- Severe COVID-19 3.5 more likely if low vitamin D (30 studies) – meta-analysis July 2021
- COVID-19 patients who had supplemented with Vitamin D were 3X less likely to enter ICU – June 2021
- Low Calcium associated with severe COVID-19 – several studies
- COVID-19 mortality 3X more likely if low vitamin D (999,179 people) – meta-analysis March 29, 2021
- COVID-19 was 2.6X more severe if very low Vitamin D (43 studies) – meta-analysis March 26, 2021
- Low Vitamin D associated with 2.7X more severe COVID-19 – 12th MA March 5, 2021
- Vitamin D supplementation fights COVID-19 – 11th meta-analysis Jan 24, 2021
- 3.7 X less likely to die of COVID-19 if supplemented with Vitamin D - meta-analysis Jan 5, 2021
- Less likely to test positive for COVID-19 if higher Vitamin D – meta-analysis Jan 6, 2021
- Vitamin D reduces COVID-19 by 80 percent - anonymous meta-analysis - Jan 5, 2021
- COVID-19 1.7X more likely to be severe if low Vitamin D - meta-analysis Oct 2020
- Low Vitamin D associated 1.8X increased risk of COVID-19 death in hospital – meta-analysis Nov 4, 2020
- Acute viral respiratory infections (RTI) reduced by Vitamin D - 20 reviews - Aug 2020
- Prudent to consider that Vitamin D has a role in COVID-19 – meta-analysis – Aug 7, 2020
- Risk of enveloped virus infection is increased 50 percent if poor Vitamin D Receptor - meta-analysis Dec 2018
- Hepatitis B patients have 2 ng lower level of Vitamin D – meta-analysis June 2019
- Influenza Vaccination not benefited by lowish levels of vitamin D – meta-analysis March 2018
Reviews
- Vitamin D supplementation reduced risk of COVID-19 ICU by 2.8 X – review of 10 reviews Feb 2022
- COVID-19 and Vitamin D (42 studies, consensus) – Oct 2021
Observe - Less likely to become infected
short URL to this section = https://is.gd/COVID_less
- 14 X less likely to have severe COVID if previously had more than 40 ng level of Vitamin D – Feb 2022
- COVID-19 patients had low levels of Zinc, Vitamin A, Vitamin D, and Vitamin C – Sept 2021
Observe - Reduced Severity/Death
MORTALITY AND Virus (automatically updated):
- Moderna report: their COVID vax caused "only" 17,751 deaths - April 2024
- COVID infection (without hospitalization) – 1.7X more likely to die in 6 months if low Vitamin D – March 2024
- Vaccines increased your risk of dying of COVID in NZ - official data - Feb 2024
- 3X increase in unspecified causes of Death (Canada 2019-2022) - Dec 2023
- Deaths after vaccination - also reported in Japan - Dec 2023
- Excess deaths after COVID vaccination - 17 countries - Sept 2023
- Excess Deaths in Australia jumped up in 2022– preprint Feb 2023
- Prevent a COVID death: 9 dollars of Vitamin D or 900,000 dollars of vaccine - Aug 2023
- Number needed to vaccinate to prevent 1 Omicron death: 30,000 for age 60-70 - Sept 2022
- COVID survival in Europe in 2020 best predicted by population-level Vitamin D (of 13 variables) – July 2022
- Elderly who had been in COVID ICU were 4X more likely to die if low vitamin D – Nov 2022
- More COVID mortality if less than 20 ng of Vitamin D (Mexico) – May 2022
- 15,000,000 excess deaths in 2 years - May 2022
- COVID death 5.2X more likely if Vitamin D deficient – May 2022
- 29 X more likely to die of COVID if less than 20 ng of Vitamin D - March 2022
- Giving Vitamin D reduced COVID Mortality– Review of 11 studies – March 2022
- 18 million excess global deaths in past 2 years: COVID plus collateral damage - Lancet March 2022
- COVID severity and death more likely if low vitamin D (Egypt this time) - March 2022
- US nursing homes are epicenters for COVID deaths (200,000) - Feb 2022
- Ivermectin taken before COVID decreased death rate by 68 percent (3,000 with Ivermectin vs 3,000 without) - Dec 24, 2021
- Increase in non-COVID deaths (ages 18-64) in Indiana, India, etc. - Jan 5, 2022
- Only 35,000 died in US of COVID who previously had been healthy
- COVID-19 mortality extrapolates to zero at 50 ng of vitamin D – 18th Meta-analysis Sept 2021
- COVID-19 patients getting 300,000 IU of Vitamin D were 5X less likely to die – Sept 2021
- Predict 2X more likely to die of COVID-19 if vitamin D Deficient (Iran 2020) – Sept 2021
- COVID-19 mortality not associated with Vitamin D (everyone had very low levels) -Sept 2021
- COVID-19 mortality for Blacks is 5X that for whites in 2 LA Hospitals - July 2021
- COVID-19 mortality was associated with vitamin D deficiency of 47 countries – July 2021
- Similar death rate for Vaccination and COVID-19 study and video – June 24, 2021
- COVID-19 death in hospital 5X more likely if low vs high vitamin D – preprint June 2021
- COVID-19 deaths 1.7X more likely if low vitamin D (even after “adjusting” for low D health problems) – May 2021
- COVID-19 deaths 1.5X less likely if more than 40 ng of vitamin D – US VA – April 2021
- Vitamin D supplementation and high levels reduce COVID-19 deaths in elderly – Review April 17, 2021
- Less COVID-19 infection, mortality in countries with higher Vitamin D (Asia in this case) – May 2021
- COVID-19 was the third-leading cause of death in the US, especially in those with dark skins - April 1, 2021
- Risk of COVID-19 death was 4.9 X higher if very low vitamin D – March 31, 2021
- COVID-19 mortality 2X higher if low Vitamin D (Mexican hospital, preprint) - March 2021
- All COVID-19 patients had low vitamin D, the lowest were more likely to die – Feb 18, 2021
- 2.7 fewer COVID-19 hospital deaths in those having more than 30 ng of vitamin D – Mayo Jan 9, 2021
- Worse COVID-19 patients got 400,000 IU of vitamin D, deaths cut in half – Jan 14, 2021
- Iranians with COVID-19 were 2.3 X more likely to die if low vitamin D – Jan 2021
- Poor COVID-19 prognosis was 6 X more likely if low vitamin D – Jan 21, 2021
- Less than 10 dollars of Vitamin D per COVID-19 life saved in Myanmar - Jan 2021
- 2.8 X fewer COVID-19 nursing home deaths if add 10,000 IU Vitamin D daily for a week (small observation)- Jan 2021
- Italian nursing home COVID-19 – 4X less likely to die if taking Vitamin D– Dec 22, 2020
- Shift workers 2X more likely to get COVID-19 (low Vitamin D) - Dec 2020
- Those getting high dose vitamin D were 7 X less likely to die of COVID-19 - Dec 11, 2020
- COVID-19 male mortality increased 3.9 X if low vitamin D – observation Nov 25, 2020
- Hospital COVID-19 observation: 7X more likely to live if more than 20 ng of vitamin D– Nov 19, 2020
- COVID-19 lung death 4X more likely in Iran if less than 25 ng of vitamin D – Oct 30, 2020
- Vitamin D of 30-40 ng fights COVID, Dr. Grimes on Liverpool Study - March 2022
- Higher vitamin D, less severe COVID and deaths in hospital (in Iran this time) – Sept 2021
Vitamin D Dosing Recommendations for COVID-19
- COVID predicted to be a pandemic that could be stopped by high dose vitamin D - Feb 2020
- FLCCC COVID guidelines now include vitamin D loading doses - Jan 2022
- Vitamin D and COVID, review of evidence, loading dose if less than 50 ng - Masterjohn Sept 2021
Short URL for this section = https://is.gd/covitamind https://is.gd/virusvitd
Title change made in Sept 2022 caused the visitor count to reset.There have actually been
| 7269 visitors, last modified 04 Jul, 2020, |
| ID | Name | Uploaded | Size | Downloads | |
|---|---|---|---|---|---|
| 13772 | German 19X.jpg | admin 29 Apr, 2020 | 54.42 Kb | 5960 | |
| 13759 | Alipio chart.jpg | admin 22 Apr, 2020 | 88.17 Kb | 13263 | |
| 13745 | table 2.jpg | admin 18 Apr, 2020 | 15.40 Kb | 4427 | |
| 13744 | COVID-19 and Vitamin D deficiency.jpg | admin 18 Apr, 2020 | 58.06 Kb | 4799 |