Overview Osteoarthritis and Vitamin D
Summary of Osteoarthritis and Vitamin D
Osteoarthritis results from narrowing of joints which are made of cartilage
Vitamin D with co-factors such as Magnesium, Calcium, Boron and vitamin K help build cartilage as well as bone
Vitamin D PREVENTS Osteoarthritis
Vitamin D TREATS Osteoarthritis - provided it has not gone so far that the bones cannot be re-built
- Vitamin D can add to bone mass - but it probably cannot re-build bone structure
Note: Osteoporosis causes bones to become fragile and prone to fracture
Osteoarthritis is a disease where damage occurs to the joints at the end of the bones
Wikipedia introduction to Osteoarthritis
"Osteoarthritis (OA) also known as degenerative arthritis or degenerative joint disease , is a group of mechanical abnormalities involving degradation of joints,[1]
including articular cartilage and subchondral bone. Symptoms may include joint pain, tenderness, stiffness, locking, and sometimes an effusion.
A variety of causes—hereditary, developmental, metabolic, and mechanical—may initiate processes leading to loss of cartilage.
When bone surfaces become less well protected by cartilage, bone may be exposed and damaged.
As a result of decreased movement secondary to pain, regional muscles may atrophy, and ligaments may become more lax.[2]"
PubMed has a good overview Which includes:
Osteoarthritis is the most common joint disorder.
Osteoarthritis is caused by 'wear and tear' on a joint.
Cartilage is the firm, rubbery tissue that cushions your bones at the joints, and allows bones to glide over one another.
Cartilage can break down and wear away. As a result, the bones rub together, causing pain, swelling, and stiffness.
Bony spurs or extra bone may form around the joint, and the ligaments and muscles around the hip become weaker and stiffer.
"Often, the cause of OA is unknown. It is mainly related to aging. The symptoms of OA usually appear in middle age. Almost everyone has some symptoms by age 70. However, these symptoms may be minor. Before age 55, OA occurs equally in men and women. After age 55, it is more common in women."
Severe cases of OA might need surgery to replace or repair damaged joints. Surgical options include:
Arthroscopic surgery to trim torn and damaged cartilage
Changing the alignment of a bone to relieve stress on the bone or joint (osteotomy)
Surgical fusion of bones, usually in the spine (arthrodesis)
Total or partial replacement of the damaged joint with an artificial joint
- (knee replacement, hip replacement, shoulder replacement, ankle replacement, elbow replacement)
See also Vitamin D Life
High dose vitamin reduced pain of fibromyalgia, osteoarthritis, and rheumatoid arthritis - July 2015
Knee osteoarthritis treated with vitamin D, weekly 50,000 IU – May 2015
Good evidence for knee osteoarthritis and vitamin D, unsure of other OA – Review March 2013
Knee osteoarthritis 2.3 X more likely to get worse if low level of vitamin D – Dec 2014
Better total hip replacement if have high vitamin D – April 2010 - better still if take vitamin D and not need replacement at all
3 more rheumatic studies found vitamin D deficiencies – June 2010
CLICK HERE for Osteoarthritis items
CLICK HERE for Rheumatoid Arthritis items
CLICK HERE for Osteoporosis items
CLICK HERE for Bone Health items
[tiki-download_file.php?fileId=1678] file
Probability of knee osteoarthritis up 50 percent if 20 ng less vitamin D – Nov 2011
Osteoarthritis twice as prevalent if vitamin D level less than 15 ng – Feb 2010
Hypothesis- Knee osteoarthritis is reduced by vitamin D increasing level of nitric oxide – Dec 2013
Hypothesis: increased bone mineral density needs protein, Ca, Mg, Vitamin D and K
Vitamin D and Boron category listing has items Seem to prevent and cure OA quickly
Vitamin D and rheumatic diseases. – Review July 2014 which shows 2X increase in OA for if low vitamin D
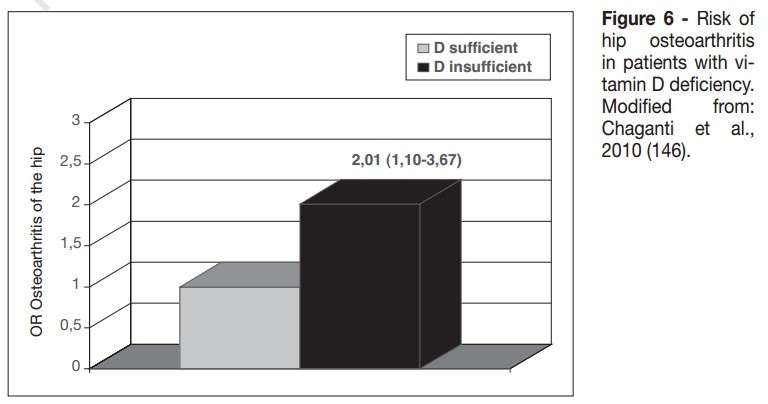
Pages listed in BOTH of the categories Osteoarthritis and Vitamin D Receptor
{category}
See also web
- CLICK HERE for Clinical Trials on knee and vitamin D - 126 trials as of Aug 2023
- included such items as: "VItamin D Effect on Osteoarthritis Study (VIDEO) 50,000 IU monthly
Intervention Trials for Osteoarthritis and Vitamin D INTERVENTION 32 trials as of Aug 2024
PubMed for osteoporosis (vitamin OR magnesium) got >13,851 hits Aug 2024
Cartilage supplement, vitamins, herbs, natural ways to improve and to have healthy tissue by Ray Sahelian,March 2014
- Nothing about vitamin D, but it is a great overview of what cartilage is and how to help it
- 10 Best Supplements for Your Joints March 2011
- 1) Glucosamine:2) Chondroitin Sulfate: 3) Omega-3, 4) SAMe: 5) TMG: 6) MSM 7) Calcium:8) Vitamin C: 9) Silicon: 10) Gelatin:
- Low Skeletal Muscle Mass in the Lower Limbs Is Independently Associated to Knee Osteoarthritis PLOS One Nov 2016
- Knee Osteoarthritis 6% more likely if low muscle mass in lower leg - seems reasonable
- Vitamin D had a smaller association - the study ignored Vitamin D cofactors such as Magnesium, Boron, etc.
- 📄 Download the PDF from Vitamin D Life
OA and Omega-3
Vitamin D and omega-3 are the only supplements which show benefit in meta-analysis – Jan 2012
Omega-3 Fatty Acids Shown to Prevent or Slow Progression of Osteoarthritis Science Daily Oct 2011
What Admin of Vitamin D Life is doing about his early indications of Osteoarthritis
During Spring/Summer of 2014 (age 68) I got sharp pain below both knees - which my Dr. diagnosed as early indication of OA.
Tried a shotgun of 7 solutions (in addition to vitamin D) and the pain went away for several weeks
Stopped all solutions and the pain returned in a few days (still had vitamin D)
Restarted with just a subset of solutions - and have had no pain at all for the past 10 days
Current solutions are
Glucosimine
Condratin
Curcumin
Magnesium Chloride liquid applied to both knees covered with DMSO ( for penetration)
Note: Magnesium: it helps muscles see Wikipedia Magnesium in biology and Magnesium deficiency (medicine)
Also see Overview Magnesium and vitamin D
I got back into Feldekrais exercises every 4 days (which I have used for 30+ years) to restore flexibility, muscle strength, and use of different muscles to accomplish the same movement.
Update April 2020
I get a tiny amount of pain in one knee about 3 times a year.
A single dose of MgCl and Boron in DMSO cream makes the tiny pain vanish overnight
Note: I have a 200 ng Vitamin D level and take Mg, Boron, Calcium etc with my morning cereal
I also do 10 things to increase the amount of vitamin D actually getting to my cells
PubMed results for osteoarthritis "vitamin d" 623 items Aug 2025
Knee pain and muscle strength helped with 50,000 IU weekly - Aug 2015
Progressive knee OA 2.4X more likely if low vitamin D - Oct 2015
25-Hydroxyvitamin D and osteoarthritis: A meta-analysis including new data
Vitamin D, race, and experimental pain sensitivity in older adults with knee osteoarthritis.
Arthritis Rheum. 2012 Dec;64(12):3926-35. doi: 10.1002/art.37687.
Association between serum vitamin D deficiency and knee osteoarthritis
Int Orthop. 2011 Nov;35(11):1627-31. doi: 10.1007/s00264-010-1186-2. Epub 2010 Dec 30. full text online
Serum levels of vitamin D, sunlight exposure, and knee cartilage loss in older adults: the Tasmanian older adult cohort study.
Arthritis Rheum. 2009 May;60(5):1381-9.
CONCLUSION: Sunlight exposure and serum 25(OH)D levels are both associated with decreased knee cartilage loss (assessed by radiograph or MRI). This is best observed using the whole range of 25(OH)D levels rather than predefined cut points and implies that achieving vitamin D sufficiency may prevent and/or retard cartilage loss in knee OA . PMID: 19404958 CLICK HERE for full article
Knee joint narrowing was found to be associated with people with low levels of vitamin D
graph from previous article

Association of low dietary vitamin K intake with radiographic knee osteoarthritis in the Japanese elderly population: dietary survey in a population-based cohort of the ROAD study.
J Orthop Sci. 2009 Nov;14(6):687-92. Epub 2009 Dec 8.
RESULTS: The prevalence of knee OA of KL >or=2 was 70.8%. Age, body mass index, and female sex were positively associated with the prevalence. Among the dietary factors, only vitamin K intake was shown to be inversely associated with the prevalence of radiographic knee OA by multivariate logistic regression analysis. The presence of joint space narrowing of the knee was also inversely associated with vitamin K intake. The prevalence of radiographic knee OA for each dietary vitamin K intake quartile decreased with the increased intake.
CONCLUSIONS: The present cross-sectional study using a population-based cohort supports the hypothesis that low dietary vitamin K intake is a risk factor for knee OA. Vitamin K may have a protective role against knee OA and might lead to a disease-modifying treatment. PMID: 19997813
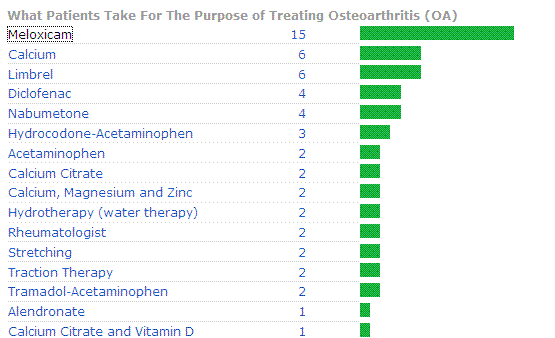
From PatientsLikeMe - Osteoarthritis
Graph of treatments people with OA use - notice frequent use of Calcium
It appears that Meloxicam = mobic
Osteoarthritis of Foot and Ankle
Nice description at http://orthoinfo.aaos.org/topic.cfm?topic=a00209 includes the following
Osteoarthritis
Many factors increase your risk for developing osteoarthritis. Because the ability of cartilage to heal itself decreases as we age, older people are more likely to develop the disease. Other risk factors include obesity and family history of the disease.
Rheumatoid Arthritis
The exact cause of rheumatoid arthritis is not known. Although it is not an inherited disease, researchers believe that some people have genes that make them more susceptible. There is usually a "trigger," such as an infection or environmental factor, which activates the genes. When the body is exposed to this trigger, the immune system begins to produce substances that attack the joint. This is what may lead to the development of rheumatoid arthritis.
Post-Traumatic Arthritis
Fractures - particularly those that damage the joint surface - and dislocations are the most common injuries that lead to this type of arthritis.
- An injured joint is about seven times more likely to become arthritic, even if the injury is properly treated.
- In fact, following injury, your body can secrete hormones that stimulate the death of your cartilage cells.
Association between serum levels of 25-hydroxyvitamin D and osteoarthritis: a systematic review - 2013
Rheumatology, Volume 52, Issue 7, Pp. 1323-1334. (July, 2013)
Yuelong Cao 1,2; Tania Winzenberg 1; Kay Nguo 1; Jianhao Lin 3; Graeme Jones 1 and Changhai Ding 1,4 [email protected]
1 Menzies Research Institute Tasmania, University of Tasmania, Hobart, Australia,
2 Research Institute of Orthopedics, Shuguang Hospital Affiliated to Shanghai University of Traditional Chinese Medicine, Shanghai, China,
3 Institute of Bone and Joint, Peking University People’s Hospital, Peking, China and 4Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, Australia.
Objective. To systematically review the evidence for association between serum 25-hydroxyvitamin D (25-(OH)D) and OA and the effect of vitamin D therapy on OA.
Methods. An English Medline, EMBASE and Cochrane Library search for vitamin D and OA from January 1980 to June 2012 was performed. Randomized controlled trials (RCTs), cohort, case–control and cross-sectional studies in adults were included. The methodological quality of the selected studies was assessed and a best-evidence synthesis was used to summarize the results due to the heterogeneity of the studies.
Results. Of the 86 evaluated articles, 2 RCTs and 13 observational studies were included in the final analyses.
The number of participants ranged from 64 to 1644 (0–100% women).
The RCTs were only reported in abstract form and showed inconsistent results, most likely due to variations in their study design.
There was insufficient or limited evidence for associations between 25-(OH)D and hand or hip OA.
For knee radiographic OA as assessed by the Kellgren and Lawrence (KL) score, there was moderate evidence showing that low levels of 25-(OH)D were associated with increased progression of radiographic OA.
Strong evidence for an association between 25-(OH)D and cartilage loss was apparent when joint space narrowing and changes in cartilage volume were considered collectively as cartilage loss.
Conclusion. 25-(OH)D appears to be implicated in structural changes of knee OA rather than symptoms, and further well-designed RCTs are required to determine whether vitamin D supplementation can slow disease progression. There is insufficient evidence for other sites.
30% to 60% less likely to get Knee Arthritis if have a high fiber diet - May 2017
- Mey York Times May 2017
- "The associations persisted even after controlling for age, sex, race, education, smoking, total calorie intake, physical activity, the intake of polyunsaturated fat and other dietary factors."
- "The mechanism is unclear, but fiber may reduce inflammation and help control weight. "
CBD reduced thumb osteoarthitis pain from 5 to 2 in just two weeks - RCT May 2022
A Randomized Controlled Trial of Topical Cannabidiol for the Treatment of Thumb Basal Joint Arthritis
Behind $31 paywall https://doi.org/10.1016/j.jhsa.2022.03.002
Described in ConsumerLab report on CBD - free 5 day trial
Excellent reviews of supplements at ConsumerLab
Associated categories: Pain chronic 8, Rheumatoid Arthritis 7, Boron 6, Intervention 4, Intervention - non daily 3
As of April 2024
Close Associations
