Vitamin D prevents Hepatitis-C and helps treat it (many studies)
Inhibition of hepatitis C virus by vitamin D - July 2021
Vitam Horm. 2021;117:227-238. doi: 10.1016/bs.vh.2021.06.006
Asako Murayama 1, Takanobu Kato 2 PDF costs $31.50 from the publisher
Until the development of direct-acting antivirals (DAAs), interferon (IFN)-based therapy had been the primary treatment strategy for patients with chronic hepatitis C, even though this therapy has a therapeutic limitations and considerable side effects. Therefore, many efforts have been made to improve the efficacy of treatment. Several clinical studies have clearly shown that supplementation with vitamin D of IFN-based therapy improves treatment efficacy. To clarify the molecular mechanisms of the effect of vitamin D on IFN-based therapy, several researchers have performed basic research with cell culture models of hepatitis C virus (HCV). Consequently, two vitamin D3 metabolites, 25-hydroxyvitamin D3 (25-(OH)D3) and 1α,25-dihydroxyvitamin D3 (1α,25-(OH)2D3), have been suggested to have anti-HCV effects. 25-(OH)D3 inhibits HCV production by suppressing infectious virus assembly through reducing apolipoprotein expression, while 1α,25-(OH)2D3 inhibits HCV production by modulating IFN signaling and/or inducing various host factors associated with the inhibition of viral genome replication. In addition, an antimicrobial peptide, LL-37, which is known to be partly regulated by vitamin D, was also reported to exhibit an anti-HCV effect by disrupting infectious viral particles directly. In conclusion, vitamin D3 supplementation improves the response rate of IFN-based therapy via the direct and/or indirect anti-HCV effects of vitamin D3 metabolites.
WHO goal: Eliminate Hepatitis - C around the world by 2030 with a $50 drug regimen (as of Feb 2024)
"Elimination requires finding infected people and rapidly treating them wherever they are — often in prisons, living in shelters or places marginalized by injecting-drug use. Of the 57 million people living with hepatitis C in low- and middle-income countries, less than a quarter know they have it. Only 1% have started taking the direct-acting antiviral regimen that’s curative in eight to 12 weeks in more than 95% of cases."
“Almost 70% of all of the hep C testing and treatment through the program is occurring in prisons now,” Grebely told me. “With the treatment scale-up, we were able to reduce the incidence of infection by half.”
New Guidelines Urge Most U.S. Adults to be Screened for Hepatitis C - March 2020
screening of all adults between the ages of 18 and 79.- New York Times
Screening for Hepatitis C Virus Infection in Adolescents and Adults US Preventive Services Task Force Recommendation Statement
"About 2.4 million Americans are living with hepatitis C"
"Hepatitis C is associated with more deaths than the other top 60 reportable infectious diseases combined "
Note: The word VITAMIN does not occur once in the recommendation
Note: The Hepatitis C test appears to range from $24 to $50
It might be better and less expensive to just give vitamin D to everyone
Hepatitis-C reduced 30% by Vitamin D (any amount) – meta-analysis Aug 2017
Efficacy of vitamin D supplementation in combination with conventional antiviral therapy in patients with chronic hepatitis C infection: a meta-analysis of randomised controlled trials.
J Hum Nutr Diet. 2017 Aug 18. doi: 10.1111/jhn.12503.
Kim HB1,2, Myung SK3,4,5, Lee YJ2,6, Park BJ2,7.
Only rarely do meta-analyses consider dose sizes or durations used in random controlled trials
📄 Download the PDF from Sci-Hub via Vitamin D Life
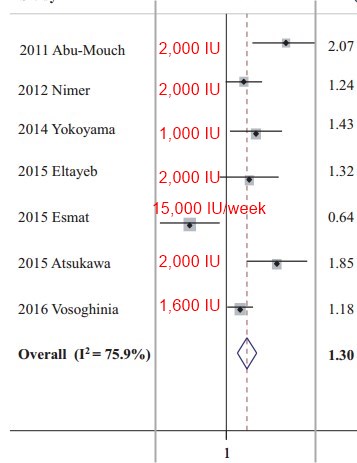
Probably would have had far better success if had used larger dose of Vitamin D - say 4,000 IU
Hepatitis C Quality of life is worse if low vitamin D - Feb 2019
Vitamin D deficiency and health-related quality of life in chronic hepatitis C.
J Viral Hepat. 2019 Feb 9. doi: 10.1111/jvh.13076.
Palazzo D1, Biliotti E1, Esvan R1, Volpicelli L1, Franchi C1, Fontanelli Sulekova L1, Spaziante M1, Santori M1, Rugova A1, Rucci P2, Taliani G1.
1 Hepatology Unit, Department of Clinical Medicine, Sapienza University of Rome, Rome, Italy.
2 Department of Biomedical and Neuromotor Sciences (DIBINEM), University of Bologna, Bologna, Italy.
📄 Download the PDF from Sci-Hub via Vitamin D Life
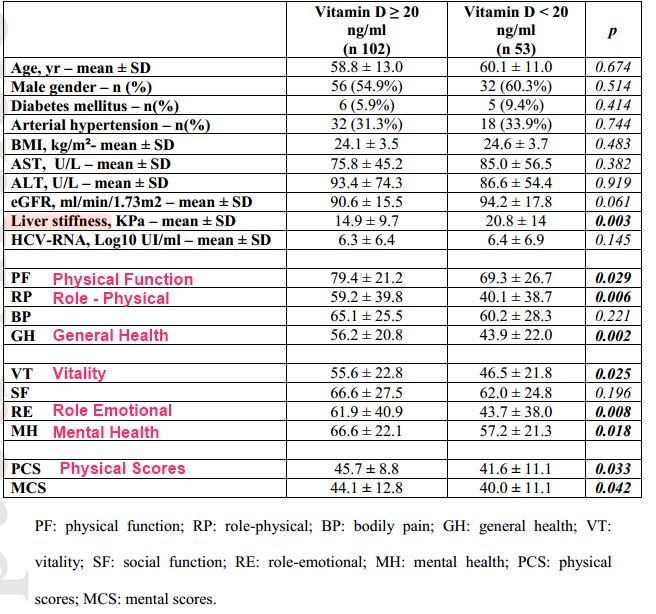
Vitamin D deficiency is common in patients with chronic liver disease, including chronic hepatitis C (CHC). However, the interplay between serum 25-hydroxy-vitamin-D (25-OH-D) and health-related-quality-of-life (HRQoL) in CHC subjects has never been investigated. The study aimed to analyze the relationship between vitamin D deficiency and HRQoL in CHC patients. One-hundred-fifty-five consecutive CHC patients completed the Health-Survey-Short-Form-36 (SF-36) and their serum 25-OH-D levels were evaluated. Vitamin D deficiency was defined as a 25-OH-D level lower than 20 ng/mL.
We identified 53 patients (34.2%) with vitamin D deficiency, who showed a mean 25-OH-D serum level of 12.5 ± 3.7 ng/mL.
Vitamin D deficient patients had significantly higher liver stiffness values compared to those with normal levels ( 20.8 ± 14 vs 14.9 ± 9.7 KPa, p=0.003). In a multivariate linear regression analysis, vitamin D deficiency was independently associated with a lower SF-36 physical-component summary score (p=0.034) and SF-36 mental-component summary score (p=0.042) after controlling for age, gender and liver stiffness.
Specifically, vitamin D deficiency was associated with 3 out of 4 physical domain s of the SF-36 [physical-function (p=0.016), role-physical (p=0.016) and general-health (p=0.002)] and 3 out of 4 mental domains [vitality (p=0.020), role-emotional (p=0.005) and mental-health (p=0.025)].
In conclusion, the present study provides novel evidence demonstrating that vitamin D deficiency can contribute to a decreased physical and mental HRQoL in CHC patients. Given that serum vitamin D levels are easy to evaluate and deficiency treatment is simple and inexpensive, clinicians should be aware of the potential multiple benefits of vitamin D supplementation in CHC patients. This article is protected by copyright. All rights reserved.
Hepatitis-C associated with low micronutrients - such as Vitamin D - June 2019
The Role of Micronutrients in the Infection and Subsequent Response to Hepatitis C Virus
📄 Download the PDF from Vitamin D Life
BACKGROUND:
Although a contributory role of vitamin D levels for the development of chronic hepatitis C has been suggested, the efficacy of vitamin D supplementation in combination with conventional antiviral therapy consisting of pegylated interferon-α (Peg-IFN-α) injection and oral ribavirin (RBV) remains unclear. We investigated its efficacy in the treatment of chronic hepatitis C via a meta-analysis of randomised controlled trials.
METHODS:
We searched PubMed, EMBASE, the Cochrane Library, ClinicalTrials.gov and the bibliographies of relevant articles to locate additional publications in September 2016. Three evaluators independently reviewed and selected eligible studies based on predetermined selection criteria.
RESULTS:
Of 522 articles meeting our initial criteria, a total of seven open-label, randomised controlled trials involving 548 participants, were included in the final analysis. Vitamin D supplementation in combination with Peg-IFN-α injection and oral RBV significantly increased the rate of viral response for hepatitis C at 24 weeks after treatment in a random-effects meta-analysis (relative risk = 1.30; 95% confidence interval = 1.04-1.62; I2 = 75.9%). Also, its significant efficacy was observed in patients with hepatitis C virus genotype 1, which is known to be refractory to antiviral therapy.
CONCLUSIONS:
In summary, we observed that additional use of vitamin D has a positive effect on sustained viral response rates of patients with chronic hepatitis C infection. However, we cannot establish the efficacy because of substantial heterogeneity, a small sample size and a low methodological quality.
Hepatitis - C description by Perplexity AI - Feb 2024
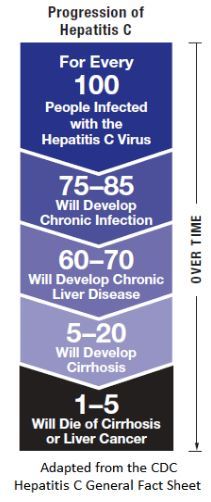
Hepatitis C is a viral infection that primarily affects the liver, caused by the hepatitis C virus (HCV). It can lead to both acute and chronic infections, with the potential to cause serious liver damage over time, including conditions such as cirrhosis and liver cancer
Transmission Hepatitis C is primarily spread through contact with blood from an infected person. Common modes of transmission include sharing needles or syringes, unsafe medical procedures like blood transfusions with unscreened blood products, and, less commonly, from mother to baby during childbirth or through sexual practices that lead to blood exposure
Symptoms Many people with hepatitis C do not exhibit symptoms, especially in the early stages of the infection. When symptoms do appear, they can include fatigue, jaundice (yellowing of the skin and eyes), dark urine, abdominal pain, loss of appetite, nausea, vomiting, and fever. Chronic hepatitis C often remains asymptomatic until it progresses to more severe liver damage
Diagnosis Diagnosis typically involves an HCV antibody test to determine if an individual has been exposed to the virus, followed by a nucleic acid test (NAT) for HCV RNA to confirm active infection. Approximately 30% of those infected with HCV spontaneously clear the infection without treatment, but they will still test positive for HCV antibodies
Treatment The treatment for hepatitis C has significantly improved over the years, with newer antiviral medications capable of curing the infection in most cases. The goal of treatment is to eradicate the virus and prevent long-term liver damage. Treatment regimens often include direct-acting antivirals (DAAs) such as sofosbuvir and daclatasvir, which can cure most people with hepatitis C within 8 to 12 weeks
Prevention Since there is no vaccine for hepatitis C, prevention focuses on reducing the risk of exposure to the virus. This includes safe injection practices, screening of blood products, and harm reduction services for people who inject drugs. It is also recommended that individuals at higher risk, such as those with HIV, men who have sex with men, and healthcare workers, undergo regular testings
Screening Recommendations Due to the asymptomatic nature of the disease, the U.S. Preventive Services Task Force recommends that all adults ages 18 to 79 years be screened for hepatitis C, even those without symptoms or known liver disease
In summary, hepatitis C is a potentially serious viral infection that can cause long-term health problems. While it often remains asymptomatic for many years, effective treatments are available that can cure the infection and prevent complications like cirrhosis and liver cancer. Regular screening and preventive measures are crucial for managing and controlling the spread of hepatitis C.
Click here for details with references, images, videos etc.
Only 25% have symptoms
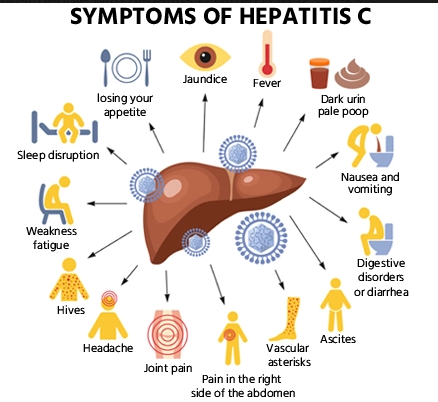
Wikipedia chart
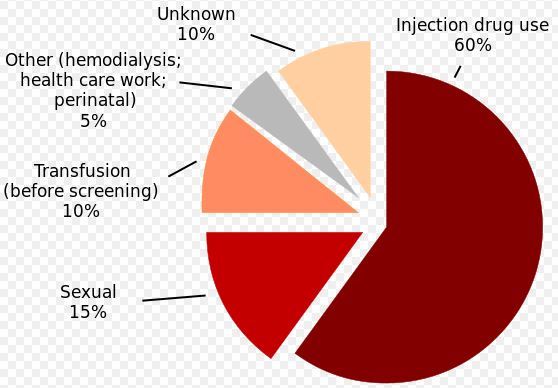
Hepatitis-C treatment greatly enhanced with 2000 IU of Vitamin D – RCT Dec 2011
Vitamin D supplementation improves sustained virologic response in chronic hepatitis C (genotype 1)-naïve patients.- 2011
World J Gastroenterol. 2011 Dec 21;17(47):5184-90. doi: 10.3748/wjg.v17.i47.5184.
Abu-Mouch S1, Fireman Z, Jarchovsky J, Zeina AR, Assy N.
AIM:
To determine whether adding vitamin D, a potent immunomodulator, improves the hepatitis C virus (HCV) response to antiviral therapy.
METHODS:
Seventy-two consecutive patients with chronic HCV genotype 1 were randomized into two groups: the treatment group (n = 36, 50% male, mean age 47 ± 11 years) received Peg-α-2b interferon (1.5 μg/kg per week) plus ribavirin (1000-1200 mg/d) together with vitamin D3 (2000 IU/d, target serum level > 32 ng/mL), and the control group (n = 36, 60% male, mean age 49 ± 7 years) received identical therapy without vitamin D. HCV-RNA was assessed by real-time polymerase chain reaction (sensitivity, 10 IU/mL). The sustained virologic response (SVR) was defined as undetectable HCV-RNA at 24 wk post-treatment.
RESULTS:
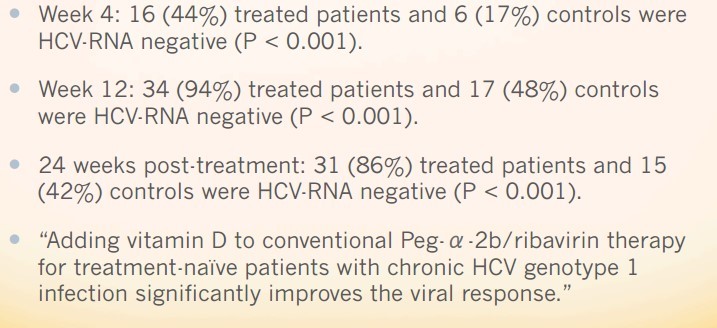
Clinical characteristics were similar in both groups. The treatment group had a higher mean body mass index (27 ± 4 kg/m² vs 24 ± 3 kg/m²; P < 0.01), viral load (50% vs 42%, P < 0.01), and fibrosis score (> F2: 42% vs 19%, P < 0.001) than the controls. At week 4, 16 (44%) treated patients and 6 (17%) controls were HCV-RNA negative (P < 0.001). At week 12, 34 (94%) treated patients and 17 (48%) controls were HCV-RNA negative (P < 0.001). At 24 wk post-treatment (SVR), 31 (86%) treated patients and 15 (42%) controls were HCV-RNA negative (P < 0.001). Viral load, advanced fibrosis and vitamin D supplementation were strongly and independently associated with SVR (multivariate analysis). Adverse events were mild and typical of Peg-α-2b/ribavirin.
CONCLUSION:
Adding vitamin D to conventional Peg-α-2b/ribavirin therapy for treatment-naïve patients with chronic HCV genotype 1 infection significantly improves the viral response.
PMID: 22215943

Evidence supporting a beneficial role of vitamin D in chronic hepatitis C. - March 2015
Letter to Editor
J Hepatol. 2015 Apr 20. pii: S0168-8278(15)00292-5. doi: 10.1016/j.jhep.2015.03.037. [Epub ahead of print]
Pang Q1, Qu K1, Zhang JY1, Liu C2.
1Department of Hepatobiliary Surgery, The First Affiliated Hospital of Xi'an Jiaotong University College of Medicine, Xi'an, China.
2Department of Hepatobiliary Surgery, The First Affiliated Hospital of Xi'an Jiaotong University College of Medicine, Xi'an, China. Electronic address: [email protected].
The Interplay between Zinc, Vitamin D and, IL-17 in Patients with Chronic Hepatitis C Liver Disease - 2015
J Immunol Res. 2015;2015:846348. doi: 10.1155/2015/846348. Epub 2015 Oct 4.
Reda R1, Abbas AA1, Mohammed M1, El Fedawy SF1, Ghareeb H1, El Kabarity RH1, Abo-Shady RA1, Zakaria D2.
OBJECTIVES:
To assess zinc (Zn) and vitamin D (Vit. D) status in chronic Hepatitis C virus- (HCV) infected patients and their relationship to interleukin- (IL-) 17 and disease severity and then investigate whether Zn and Vit. D3 modulate IL-17 expression in chronic HCV patients.
METHODS:
Seventy patients and fifty healthy subjects were investigated. Serum levels of Zn, Vit. D, and IL-17 were assessed in the patients group and subgroups. Patients lymphocytes were activated in vitro in the presence or absence of Zn or Vit. D3 and then intracellular IL-17 production was assessed using flow cytometry.
RESULTS:
Zn and Vit. D were significantly decreased in HCV patients. Increasing disease severity leads to more reduction in Zn level opposed by increasing IL-17 level. Zn potently reduced IL-17 production in a dose-related fashion; however it did not exert any toxic effects. Although Vit. D apparently increases IL17 expression , it is unclear whether it is due to its toxic effect on cell count or lack of definite association between Vit. D and both IL-17 and disease severity.
CONCLUSIONS:
This study demonstrates that Zn modulates IL-17 expression and provides a rationale for evaluating this compound as a supplementary agent in the treatment of chronic HCV.
PMID: 26504859 PMCID: PMC4609465 DOI: 10.1155/2015/846348
📄 Download the PDF from Vitamin D Life
Vitamin D status and viral response to therapy in hepatitis C infected children - 2015
World J Gastroenterol. 2015 Jan 28;21(4):1284-91. doi: 10.3748/wjg.v21.i4.1284.
Eltayeb AA1, Abdou MA1, Abdel-aal AM1, Othman MH1.
AIM:
To study the frequency of vitamin D deficiency in patients with hepatitis C virus (HCV) infection and to evaluate the role of vitamin D supplementation in improving antiviral therapy.
METHODS:
Sixty-six children aged from 7-14 years (mean ± SD, 11.17±2.293) diagnosed with HCV infection were matched to 28 healthy controls. Serum levels of 25 (OH) D3, calcium, phosphorus, alkaline phosphatase and plasma level of parathormone were measured. Quantitative PCR for HCV was performed Bone density was determined by dual energy X-ray absorptiometry. All cases received conventional therapy, and only 33 patients received vitamin D supplementation.
RESULTS:
Children with HCV showed significantly increased levels of HCV RNA (P<0.001), parathormone (P<0.01) and decreased vitamin D levels (P<0.05) (33.3% deficient and 43.3% insufficient) compared with controls. Abnormal bone status (Z score -1.98±0.75) was found in ribs, L-spine, pelvis and total body. Cases treated with vitamin D showed significant higher early (P<0.04) and sustained (P<0.05) virological response. There was a high frequency of vitamin D deficiency among the Egyptian HCV children, with significant decrease in bone density. The vitamin D level should be assessed before the start of antiviral treatment with the correction of any detected deficiency.
CONCLUSION:
Adding vitamin D to conventional Peg/RBV therapy significantly improved the virological response and helped to prevent the risk of emerging bone fragility.
PMID: 25632203 PMCID: PMC4306174 DOI: 10.3748/wjg.v21.i4.1284
📄 Download the PDF from Vitamin D Life
Reduced Hepatitis C response in those with higher levels of vitamin D - Aug 2014
Serum 25(OH)D3 levels affect treatment outcomes for telaprevir/peg-interferon/ribavirin combination therapy in genotype 1b chronic hepatitis C.
Dig Liver Dis. 2014 Aug;46(8):738-43. doi: 10.1016/j.dld.2014.05.004. Epub 2014 May 29.
Atsukawa M1, Tsubota A2, Shimada N3, Abe H4, Kondo C5, Itokawa N5, Nakagawa A5, Iwakiri K5, Kawamoto C6, Aizawa Y4, Sakamoto C6.
BACKGROUND:
Close relationships between chronic hepatitis C and vitamin D levels have been reported. For genotype 1b infection, the current standard of care is pegylated interferon/ribavirin therapy combined with a protease inhibitor. The present study analyzed the relationship between outcomes of triple therapy and serum 25(OH)D3 levels.
METHODS:
Factors contributing to sustained virological response were investigated in 177 patients with chronic hepatitis C who received telaprevir-based triple therapy in this prospective study.
RESULTS:
The sustained virological response rate was 86.9% in patients with 25(OH)D3 levels of >18 ng/ml; this was higher than the 66.7% in patients with 25(OH)D3 levels of ≤ 18 ng/ml (P=0.003). 25(OH)D3 levels and IL28B genotype were identified as significantly independent factors contributing to sustained virological response. The sustained virological response rate did not differ according to 25(OH)D3 levels in patients with the IL28B major genotype. The sustained virological response rate was 64.9% in patients with the IL28B minor genotype and 25(OH)D3 levels of >18 ng/ml, and was 38.5% in those with decreased 25(OH)D3 levels (P=0.045).
CONCLUSIONS:
In triple therapy, 25(OH)D3 levels were an independent factor contributing to sustained virological response. Of particular note, the sustained virological response rate was significantly lower in patients with the IL28B minor genotype.
Publisher wants $36 for the PDF
Vitamin D reduced Hepatitis C in Hepatocellular Carcinoma Cell Line - May 2019
Int J Mol Sci. 2019 May 13;20(9). pii: E2367. doi: 10.3390/ijms20092367.
25-Hydroxyvitamin D Inhibits Hepatitis C Virus Production in Hepatocellular Carcinoma Cell Line by a Vitamin D Receptor-Independent Mechanism
Ravid A1, Rapaport N2, Issachar A3, Erman A4, Bachmetov L5, Tur-Kaspa R6,7,8, Zemel R9.
📄 Download the PDF from Vitamin D Life
Previously, we have reported that the active vitamin D metabolite, calcitriol and vitamin D3 (cholecalciferol), both remarkably inhibit hepatitis C virus production. The mechanism by which vitamin D3 exerts its effect is puzzling due to the low levels of calcitriol produced in vitamin D3-treated Huh7.5 cells. In this study, we aimed to explore the mechanism of vitamin D3 anti-hepatitis C virus effect. We show that vitamin D3 activity is not mediated by its metabolic conversion to calcitriol, but may be due to its primary metabolic product 25(OH)D3. This is inferred from the findings that 25(OH)D3 could inhibit hepatitis C virus production in our system, and that adequate concentrations needed to exert this effect are produced in Huh7.5 cells treated with vitamin D3. Using the CRISPR-Cas9 editing technology to knockout the vitamin D receptor, we found that the antiviral activity of vitamin D3 and 25(OH)D3 was not impaired in the vitamin D receptor knockout cells. This result indicates that 25(OH)D3 anti-hepatitis C virus effect is exerted by a vitamin D receptor-independent mode of action. The possibility that vitamin D3 and 25(OH)D3, being 3β-hydroxysteroids, affect hepatitis C virus production by direct inhibition of the Hedgehog pathway in a vitamin D receptor-independent manner was ruled out. Taken together, this study proposes a novel mode of action for the anti-hepatitis C virus activity of vitamin D3 that is mediated by 25(OH)D3 in a vitamin D receptor-independent mechanism.
Ribavirin aids in treatment of Hepatitis - C before it can cause liver cancer - April 2022
See also Web
Vitamin D deficiency in hepatitis C virus infection: what is old? what is new? - July 2018 doi: 10.1097/MEG.0000000000001134.
25-Vitamin D levels in chronic hepatitis C infection: association with cirrhosis and sustained virologic response - 2017 doi: 10.20524/aog.2017.0120 free PDF
Vitamin D deficiency and hepatitis viruses-associated liver diseases: A literature review Jan 2018 free PDF
Vitamin D deficiency is a risk factor for infections in patients affected by HCV-related liver cirrhosis - Oct 2017 doi: 10.1016/j.ijid.2017.07.026 free PDF
Hepatitis C: 25 Years From Discovery to Cure Medscape nov 2014
- Calcidiol (a form of vitamin D) is better than the expensive solution, which 25 years to develope
- Vitamin D status and viral response to therapy in hepatitis C infected children. Jan 2015
- Egypt. Children getting the 2,000 IU vitamin D added to therapy had a higher early and sustained virological response
- This study seems very similar to the one on this page - but different authors
- 📄 Download the PDF from Vitamin D Life.
- 2.5X increased risk of Liver Cancer if have had Hepatitis-C April 2015
- prostate cancers also increased by 2X, probably due to low vitamin D
- It is extremely important to restore vitamin D levels if they become low
- See: Diseases that may be related via low vitamin D
- Harvoni, a Hepatitis C Drug From Gilead, Wins F.D.A. Approval NYT Oct 2014
- New drug costs only $63,000 for 8 weeks. (vs perhaps $10 for Vitamin D)
- Costly to Treat, Hepatitis C Gains Quietly in U.S. NYT July 2015
- estimate that 3 million in US have Hepatitis-C (90% unaware that they have it because it rarely has symptoms)
- 15,000 deaths in 2013
- $50 million spent by Kentucky in 2014 on Hepatitis drugs (7% of their total Medicad budget)
- This $50 million treated just 861 of 16,000 people in Kentucky with Hepatitis-C
- No mention of Vitamin D2
- Hepatitis C virus Gale Labs has the following summary
Adding Vitamin D2 after after Hepatitis-C antiviral did not help RVT Feb 2021
"Effect of vitamin D supplementation in patients with chronic hepatitis C after direct-acting antiviral treatment: a randomized, double-blind, placebo controlled trial"
Hepatitis C not helped by Vitamin D2 - RCT Feb 2021, FREE PDF doi: 10.7717/peerj.10709. eCollection 2021
Vitamin D Life pages with HEPATITIS in title (23 as of April 2022)
This list is automatically updated
{LIST()}
