Crohn’s Disease associated with lower Vitamin D - meta-analysis
Vitamin D deficiency associated with Crohn’s disease and ulcerative colitis: a meta-analysis of 55 observational studies
Journal of Translational Medicine volume 17, Article number: 323 (2019)
Xi-Xi Li, Yang Liu, Jie Luo, Zhen-Dong Huang, Chao Zhang & Yan Fu
📄 Download the PDF from Vitamin D Life
Most of the studies found that people with Chron's Disease had lower levels of Vitamin D
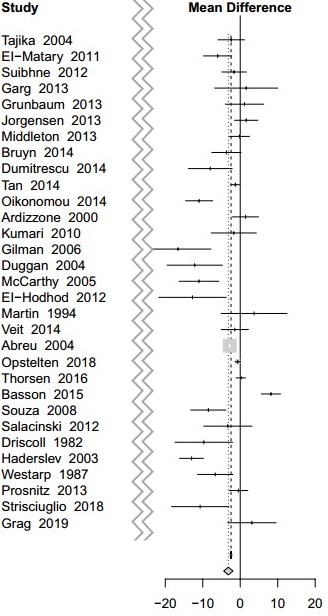
Purpose: To investigate the association of serum levels of 25(OH)D and 1,25(OH)2D3 in healthy and non-healthy controls with Crohn’s disease (CD) and ulcerative colitis (UC).
Methods: Three electronic databases: PubMed, EMbase and EBSCO host CINAHL, were searched for observational studies to measure the relationship between serum levels of vitamin D (VitD) and CD (or UC).
Results
Fifty-five studies were included in the meta-analysis. We found that mean serum 25(OH)D levels in patients with CD were significantly lower than those in healthy controls (MD: − 3.17 ng/mL; 95% CI − 4.42 to − 1.93). Results from the meta-analysis examining 1,25(OH)2D3 levels in Crohn’s patients revealed higher levels in the CD group than in healthy (MD: 3.47 pg/mL; 95% CI − 7.72 to 14.66) and UC group (MD: 5.05 pg/mL; 95% CI − 2.42 to 12.52). Serum 25(OH)D levels were lower in the UC group than in the healthy control group (MD: − 2.52 ng/mL; 95% CI − 4.02 to − 1.02). In studies investigating the level of 1,25(OH)2D3 in UC and healthy control groups, the level of 1,25(OH)2D3 in the UC groups were found to be higher than that in the control groups (MD: 3.76 pg/mL; 95% CI − 8.36 to 15.57). However, the 1,25(OH)2D3 level in patients with UC was lower than that in CD groups (MD: − 6.71 pg/mL; 95% CI − 15.30 to 1.88). No significant difference was noted between CD patients and UC patients in terms of average serum 25(OH)D levels.
Conclusions
This study found that VitD levels were inversely related to CD and UC. Serum levels of 25(OH)D were lower in patients with CD and UC than in healthy people, and more than half of the patients had insufficient vitamin D levels. The serum level of 1,25(OH)2D3 in both the CD and UC groups was higher than that in healthy people
